Is Your Battle Buddy at Risk? How to Spot Suicidal Ideation and The VA’s Push for Psychedelic Therapy
Written by: David Connell
The mental health crisis among U.S. military veterans is an ongoing and urgent issue, with post-traumatic stress disorder (PTSD) and suicide rates continuing to rise. According to the 2024 National Veteran Suicide Prevention Annual Report, 6,407 veterans died by suicide in 2022, with an average of 17.6 veteran suicides per day. Despite representing only 6.4% of the U.S. population, veterans account for 20% of all suicides in the country. PTSD remains a leading contributor, affecting nearly 25% of veterans who die by suicide. Traditional treatments, including selective serotonin reuptake inhibitors (SSRIs) and cognitive behavioral therapy, have helped some veterans but have proven inadequate for many. New approaches, including psychedelic-assisted therapy, are offering hope where conventional treatments have fallen short.
The Reality of Living With PTSD
Post-traumatic stress disorder (PTSD) is a psychiatric disorder that develops in response to trauma, often characterized by intrusive memories, severe anxiety, emotional numbness, and hypervigilance. Research shows that veterans with PTSD are significantly more likely to die by suicide, particularly those who have survived multiple combat wounds or traumatic brain injuries (TBIs). The suicide rate for veterans aged 18 to 34 was 47.6 per 100,000 in 2022, making them one of the highest-risk groups. Factors such as social isolation, chronic pain, and substance abuse further complicate recovery efforts, highlighting the need for alternative therapies.
For many veterans, PTSD is not just a collection of symptoms, it is a daily battle. The condition can manifest in flashbacks, nightmares, emotional numbness, irritability, and an overwhelming sense of hypervigilance, making it difficult to feel safe or at peace. Loud and sudden sounds, crowded spaces, or even an unexpected touch can trigger a flood of distressing memories. Many veterans find themselves withdrawing from loved ones, struggling to maintain relationships, or experiencing waves of guilt and shame, particularly if they lost fellow service members in combat.
Sleep is often one of the first things to suffer. Insomnia and night terrors leave many veterans exhausted and on edge, fueling anxiety and depression. This, combined with difficulty concentrating and an increased startle response, can make it hard to hold down a job or even complete daily tasks. Over time, PTSD can erode a veteran’s sense of identity, leaving them feeling disconnected from civilian life and questioning their worth.
Unfortunately, veterans often hesitate to seek help due to the stigma surrounding mental health treatment in military culture. Some fear being seen as weak, while others have had negative experiences with traditional talk therapy or medication. Without intervention, PTSD can intensify, leading to depression, substance use, self-destructive behaviors, and, tragically, suicidal thoughts.
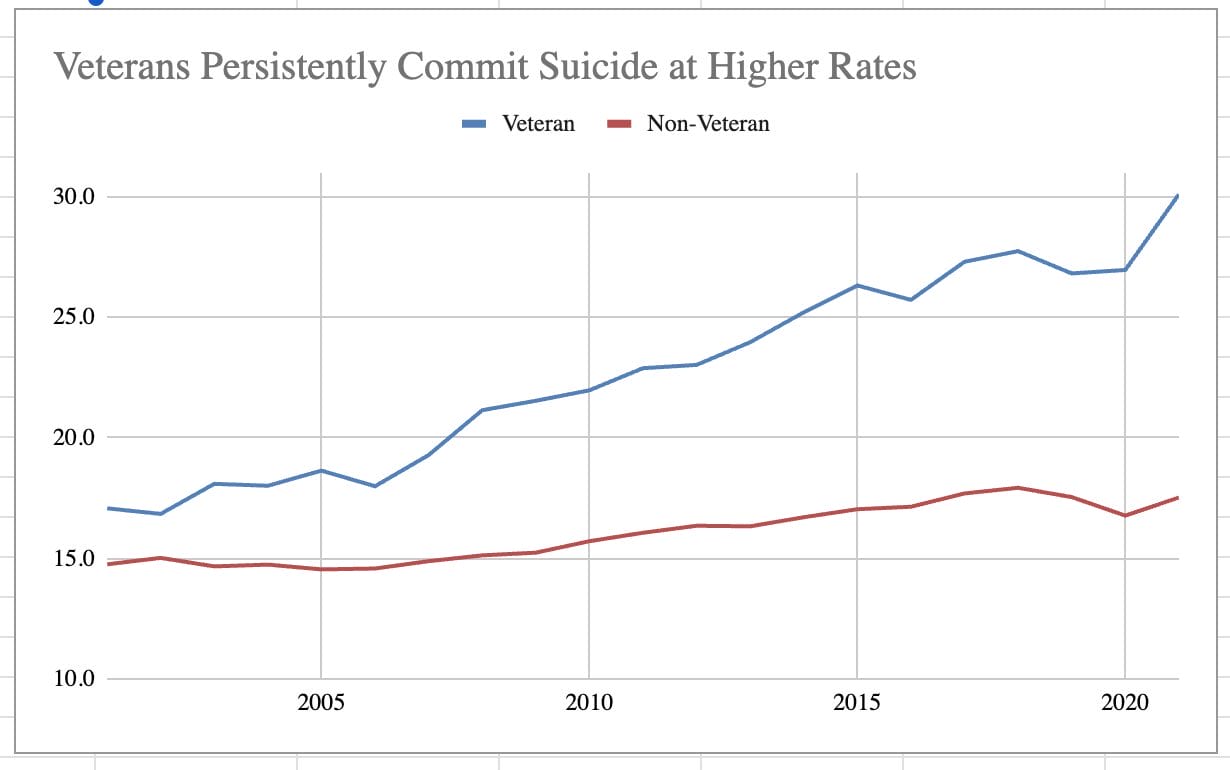

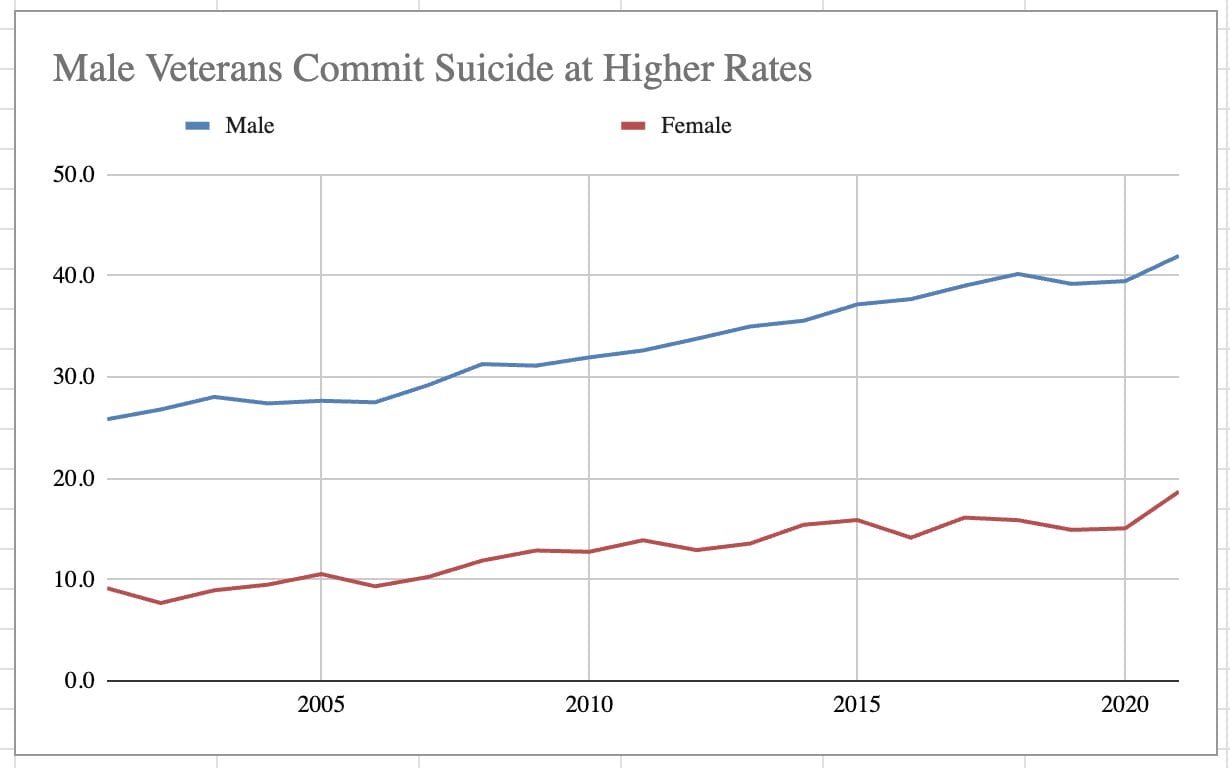

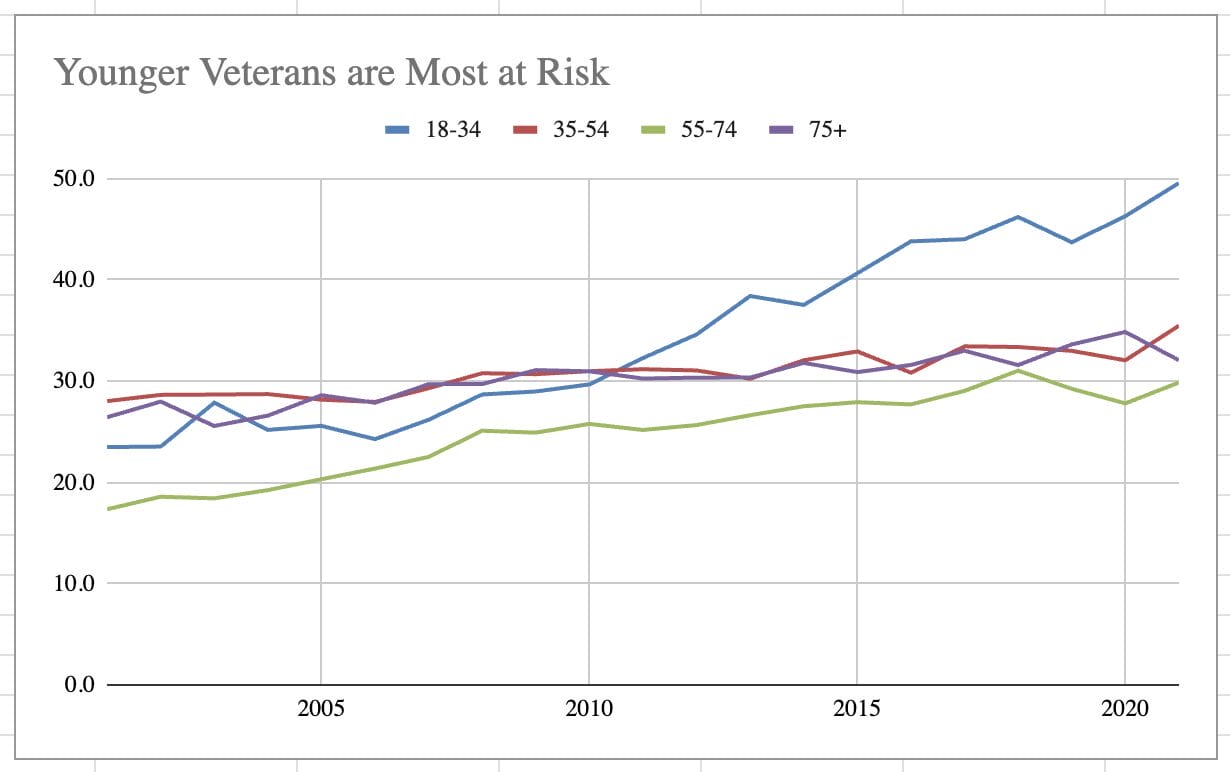

Analysis of VA suicide data shows that veterans have persistently committed suicide at higher rates, that this gap has widened in recent years, and that men and younger veterans are most at risk.
Recognizing the Warning Signs of Suicidality
Veterans often don’t openly talk about suicidal thoughts, making it crucial for family members and friends to recognize subtle but significant warning signs. While no single behavior guarantees that a veteran is at risk, some common red flags include:
- Expressing feelings of hopelessness or being a burden (“I don’t see the point anymore,” “You’d be better off without me”)
- Withdrawing from loved ones and isolating themselves
- Increased substance use, particularly alcohol, amphetamines or opioids
- Sudden mood swings, particularly from deep despair to an unusual sense of calm
- Giving away prized possessions or making arrangements as if preparing for an end
- Engaging in reckless behavior, such as excessive speeding or picking fights
- Drastic changes in sleep patterns—either sleeping too much or not at all
- A history of previous suicide attempts or self-harm
Some veterans may not explicitly say they are considering suicide, but their behavior can speak volumes. Changes in demeanor, avoidance of their favorite activities, or frequent talk of death, even in a joking manner, should be taken seriously. If a veteran expresses any of these signs, check in with them, offer support, and connect them with resources before it’s too late.
Bridging the Gap to Effective Treatment
Despite ongoing efforts by the Department of Defense, Department of Veterans Affairs (VA), and family members, many veterans continue to struggle with severe mental health conditions. While traditional treatments such as antidepressants and talk therapy help some, they remain insufficient for many with post-traumatic stress disorder (PTSD), particularly combat veterans. With suicidality rates still high and frontline treatments often falling short, interest in alternative approaches like psychedelic-assisted therapy has grown, offering a complementary tool in psychiatric care.
Emerging clinical research highlights the potential of substances like MDMA (also known as Molly or Ecstasy), psilocybin (the pro-drug found in magic mushrooms), ibogaine, and ketamine in helping veterans process trauma, alleviate depression, and regain a sense of purpose. Psychedelic-assisted therapy is not yet widely available within the VA system, but interest is increasing. The VA has begun taking steps to better understand these therapies, funding research and facilitating discussions about their role in veteran care. While challenges remain, there is growing momentum toward integrating these treatments where appropriate.
MDMA, in particular, has shown significant promise. A 2023 phase III clinical trial found that veterans who underwent MDMA-assisted therapy experienced a 71.2% reduction in PTSD symptoms, with nearly half reaching full remission. Unlike SSRIs, which often require long-term use, MDMA therapy consists of a few guided sessions that allow veterans to process traumatic memories in a safe and structured environment. In 2024 the VA announced $1.5 million to fund its first study on MDMA-assisted therapy for PTSD and alcohol use disorder (AUD), signaling a willingness to explore these treatments further.
Psilocybin, the psychoactive compound in magic mushrooms, has also demonstrated therapeutic potential. Studies suggest that psilocybin-assisted therapy promotes neuroplasticity and emotional processing, allowing veterans to engage with trauma in a meaningful way. Early research indicates that a single high-dose psilocybin session can provide long-term symptom relief. Recognizing this, the VA has issued a request for applications to study the potential of psychedelic compounds in treating PTSD and depression, marking a significant step toward evidence-based evaluation of these therapies.
Ibogaine, a psychoactive alkaloid known for its potential in treating PTSD and traumatic brain injuries, is another area of interest. A 2024 study on magnesium-assisted ibogaine therapy (MISTIC) found notable improvements in PTSD, depression, and anxiety symptoms among special operations veterans. However, ibogaine carries certain cardiovascular risks, and more research is needed to determine the safest clinical applications. The VA is monitoring this research closely while working to ensure veterans have access to the best available treatment options.
Regulatory hurdles remain a challenge. While MDMA-assisted therapy was on track for FDA approval in 2024 those efforts were temporarily derailed when the FDA rejected Lykos Therapeutics new drug application due to concerns over study design flaws, data integrity, and other concerns, as well as the need for an additional phase III trial to further assess safety and efficacy. Furthermore, psilocybin and ibogaine are still classified as Schedule I substances, limiting their availability. However, the VA is engaged in ongoing research efforts and dialogue around these treatments. Veteran advocacy groups, including the Heroic Hearts Project, are also playing a critical role in expanding access by connecting veterans with psychedelic therapy programs and supporting further study. By working together, researchers, policymakers, and veteran organizations are laying the groundwork for a more inclusive approach to care.
The VA’s approach to PTSD treatment continues to evolve as new evidence emerges. Current VA protocols emphasize prolonged exposure therapy and SSRIs, which remain essential tools, but there is recognition that additional options may be needed. The VA’s involvement in psychedelic research, combined with increasing interest from private clinics and nonprofit organizations, signals a shift toward a more comprehensive and flexible mental health strategy. The Department of Defense (DoD) is also taking steps in this direction with the creation of the DoD Psychedelic Treatment Research Clinical Trial Award. This program has set aside $9.8 million in funding for studies and clinical trials involving psychedelic medicine.
Psychedelic-assisted therapy is not a cure-all, but when combined with traditional mental health treatments, structured therapy, and veteran support networks, it offers a promising tool for addressing the root causes of treatment-resistant PTSD, substance use disorder, and depression. Ensuring proper screening, set, and setting remains crucial for maximizing benefits while minimizing risks. As research progresses, the hope is that these therapies will be integrated in ways that complement existing treatments and provide veterans with more options for effective healing.
Veterans have made immense sacrifices, and they deserve access to every possible avenue for effective treatment. With suicide rates still at crisis levels, it is essential to prioritize evidence-based care—including psychedelic-assisted therapy where appropriate. The road ahead requires collaboration between the VA, medical researchers, and veteran advocacy groups. By expanding research, improving access, and keeping veteran needs at the center of the conversation, the goal is to create a mental health system that truly serves those who have served.
David Connell is a U.S. Air Force veteran with 14 years of combined service in active duty and the reserves, including multiple deployments to Afghanistan, Ethiopia, Djibouti, and beyond. A dedicated writer and researcher, he is the author of Cooking with Magic: The Psilocybin Cookbook and formerly served as Senior Editor for Psychedelics.com. David is currently pursuing a master’s degree in Psychedelic and Consciousness Studies at the University of Ottawa, where he explores the intersection of psychedelics, psychology, and the human condition.
Sources:
Cherian, K. N., Keynan, J. N., Anker, L., Faerman, A., Brown, R. E., Shamma, A., et al. (2024). Magnesium–Ibogaine Therapy in Veterans With Traumatic Brain Injuries. Nature Medicine, 30(2), 373–381. doi: 10.1038/s41591-023-02705-w
Davis, A. K., Barrett, F. S., May, D. G., Cosimano, M. P., Sepeda, N. D., Johnson, M. W., Finan, P. H., & Griffiths, R. R. (2020). Effects of Psilocybin-Assisted Therapy on Major Depressive Disorder: A Randomized Clinical Trial. JAMA Psychiatry, 78(5), 481–489. doi: 10.1001/jamapsychiatry.2020.3285
Department of Veterans Affairs. (2024). 2024 National Veteran Suicide Prevention Annual Report. Office of Suicide Prevention. Retrieved from https://www.mentalhealth.va.gov/docs/data-sheets/2023/2023-National-Veteran-Suicide-Prevention-Annual-Report-FINAL-508.pdf
Department of Veterans Affairs. (2023). Suicide & PTSD Statistics. Retrieved from https://www.mentalhealth.va.gov/suicide_prevention/data.asp
Eaton, Erica, Christy Capone, Brian J. Gully, Zoe E. Brown, Mollie Monnig, Michael S. Worden, Robert M. Swift, and Carolina L. Haass-Koffler. “Design and methodology of the first open-label trial of MDMA-assisted therapy for veterans with post-traumatic stress disorder and alcohol use disorder: Considerations for a randomized controlled trial.” Contemporary Clinical Trials Communications, vol. 41, 2024, p. 101333. Elsevier, doi:10.1016/j.conctc.2024.101333.
Mitchell, J. M., Ot’alora G., M., van der Kolk, B., Shannon, S., Bogenschutz, M., Gelfand, Y., et al. (2023). MDMA-Assisted Therapy for Moderate to Severe PTSD: A Randomized, Placebo-Controlled Phase 3 Trial. Nature Medicine, 29(10), 2473–2480. doi: 10.1038/s41591-023-02565-4VA National Center for PTSD. (2023). PTSD and Suicide. Retrieved from https://www.ptsd.va.gov/understand/related/suicide_ptsd.asp
Previous Post
Flying to New Heights: Kegan’s Story Part 2
